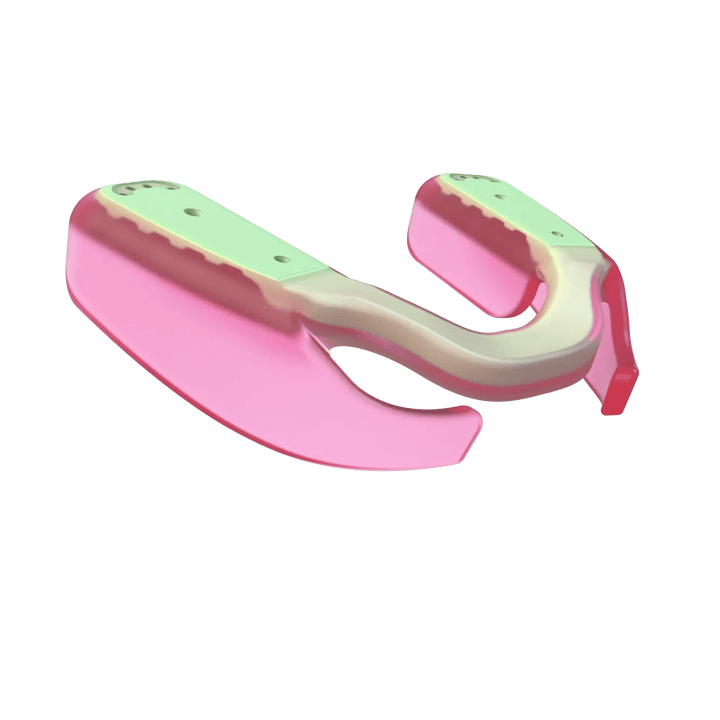Deep Sleep Explained: What Actually Interrupts Physical Recovery
Deep sleep is where physical recovery happens. It is the stage of sleep most closely tied to tissue repair, immune function, and the hormonal processes that help your body adapt to stress.
Yet many people spend enough time asleep and still struggle to feel physically restored. Training feels harder. Soreness lingers. Recovery metrics stay suppressed.
The reason is usually not a lack of sleep. It is repeated interruption of deep sleep.
What Deep Sleep Actually Does
Deep sleep, sometimes called slow wave sleep, is the most physically restorative stage of sleep.
During deep sleep:
-
Growth hormone release increases
-
Tissue repair accelerates
-
Inflammation regulation improves
-
The nervous system downshifts
-
Energy stores begin replenishing
This stage typically occurs earlier in the night, but it depends on continuity. Deep sleep needs sustained calm conditions to do its work.
When deep sleep is interrupted, the body does not simply pick up where it left off. Recovery becomes incomplete.
Why Deep Sleep Is So Vulnerable
Deep sleep requires the nervous system to fully disengage from alertness.
That means:
-
Low heart rate
-
High parasympathetic activity
-
Stable breathing
-
Minimal sensory input
If any of those signals change, the brain shifts you into lighter sleep. You may not wake up, but the recovery process is paused.
This is why deep sleep can quietly disappear without you realizing it.
The Most Common Causes of Interrupted Deep Sleep
Many factors can interfere with deep sleep, but only a few account for most disruptions.
Nervous system load
Stress, heavy training, illness, and under recovery raise baseline alertness. This makes it harder to sustain deep sleep.
Temperature instability
If the body cannot maintain a stable core temperature, deep sleep becomes harder to hold.
Breathing inconsistency
Subtle instability in breathing is one of the most common and overlooked disruptors.
When airflow becomes inconsistent, the brain increases alertness just enough to stabilize breathing. That shift pulls you out of deep sleep without waking you fully.
Why Breathing Plays Such a Big Role
During deep sleep, muscle tone decreases significantly. This includes muscles that help support airway structure and tongue position.
When muscle support drops:
-
Airflow relies more on anatomy and reflexes
-
Breathing becomes more sensitive to positioning
-
Small disruptions trigger protective responses
These responses are automatic. The brain prioritizes stable breathing over staying in deep sleep.
Over the course of the night, repeated interruptions can dramatically reduce total deep sleep time.
What This Looks Like in Your Data
Wearable data often shows the impact of interrupted deep sleep clearly.
Common patterns include:
-
Lower than expected deep sleep percentage
-
Fragmented deep sleep periods
-
Elevated sleep stress
-
Suppressed HRV
-
Higher sleeping heart rate
People often describe this as sleeping long enough but feeling physically flat or sore the next day.
Why Athletes and Active People Feel This First
Deep sleep is especially important for people who place high physical demands on their bodies.
Training creates stress that must be resolved during sleep. If deep sleep is interrupted, adaptation slows.
This can show up as:
-
Persistent muscle soreness
-
Plateaued performance
-
Increased fatigue
-
Longer recovery times between sessions
When recovery demands are high, the margin for deep sleep disruption becomes smaller.
Why Sleep Habits Alone May Not Protect Deep Sleep
Good sleep habits create the conditions for deep sleep, but they do not guarantee it.
Once you are asleep, the body responds to physical signals. If breathing becomes unstable or the nervous system senses stress, deep sleep is interrupted regardless of bedtime routines.
This is why people can do everything right and still struggle with physical recovery.
Where Airway Support Fits In
Protecting deep sleep often requires improving the physical environment the body experiences during sleep.
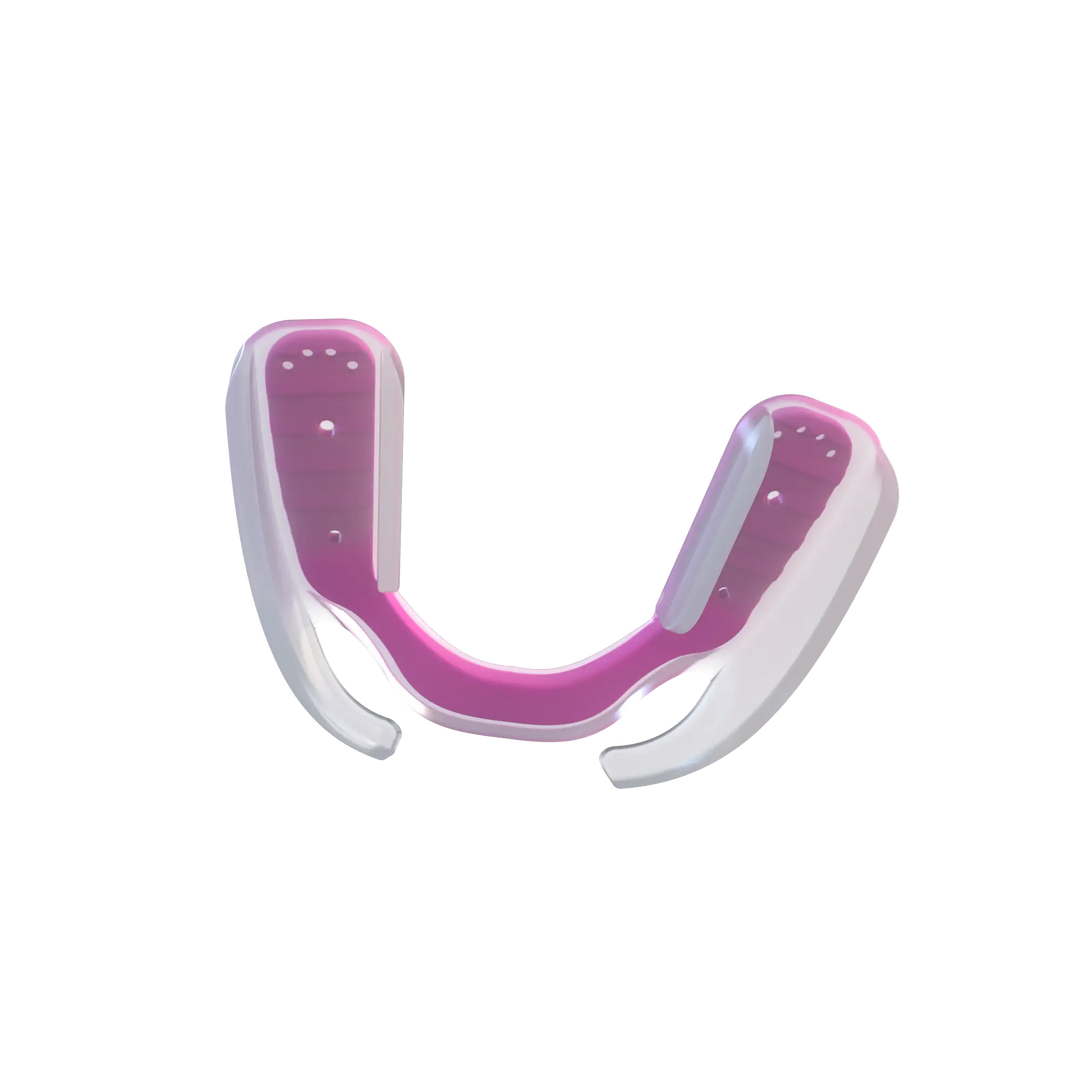
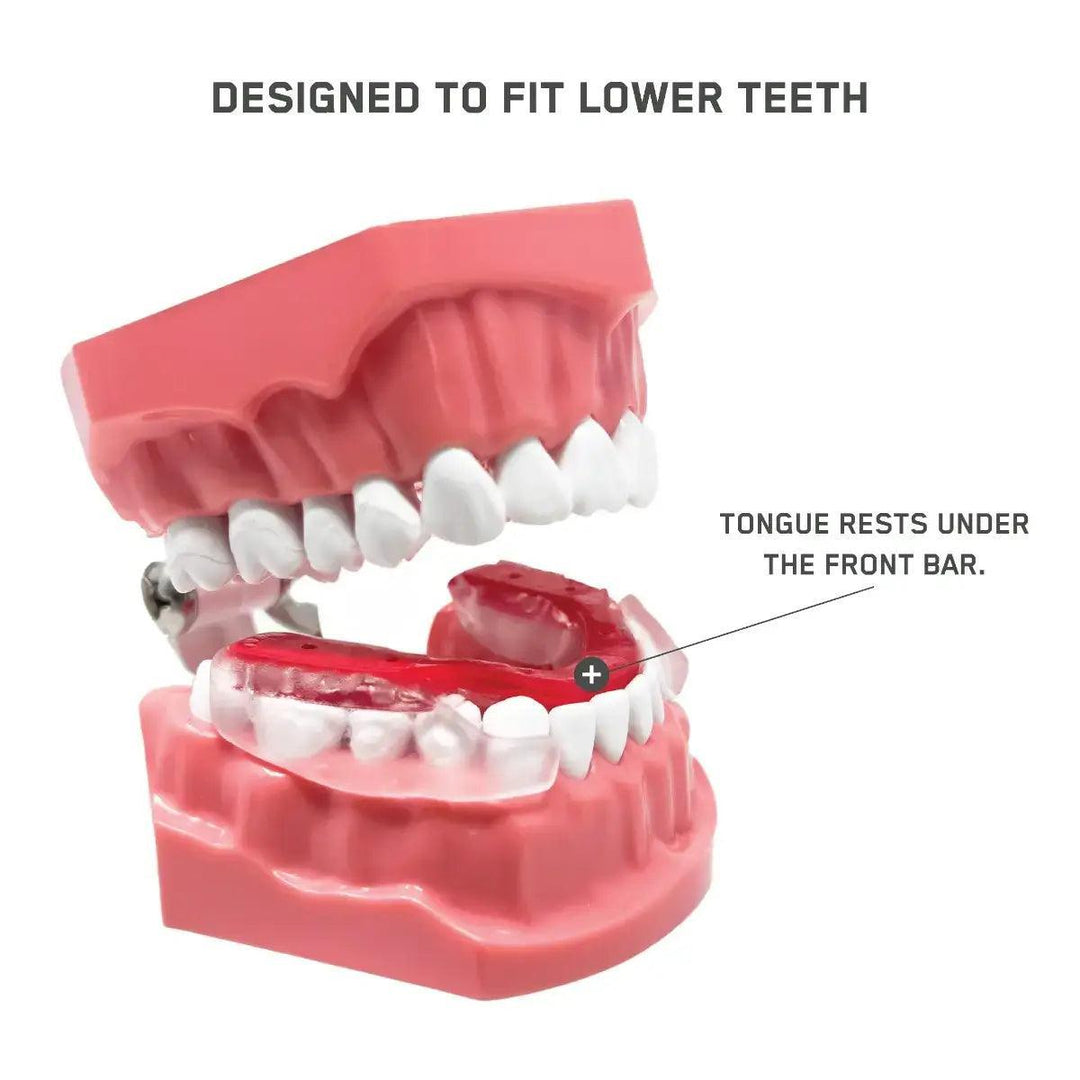
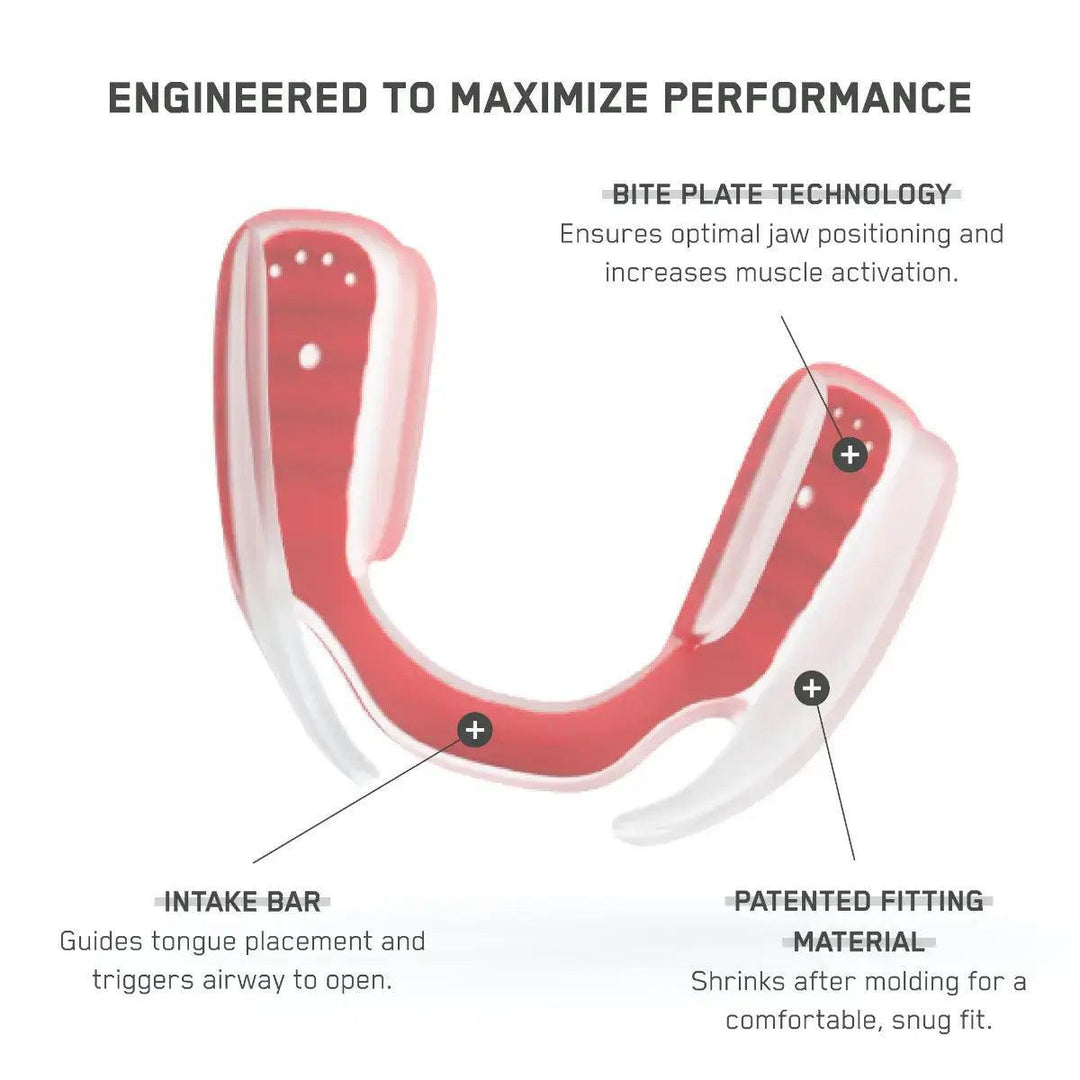
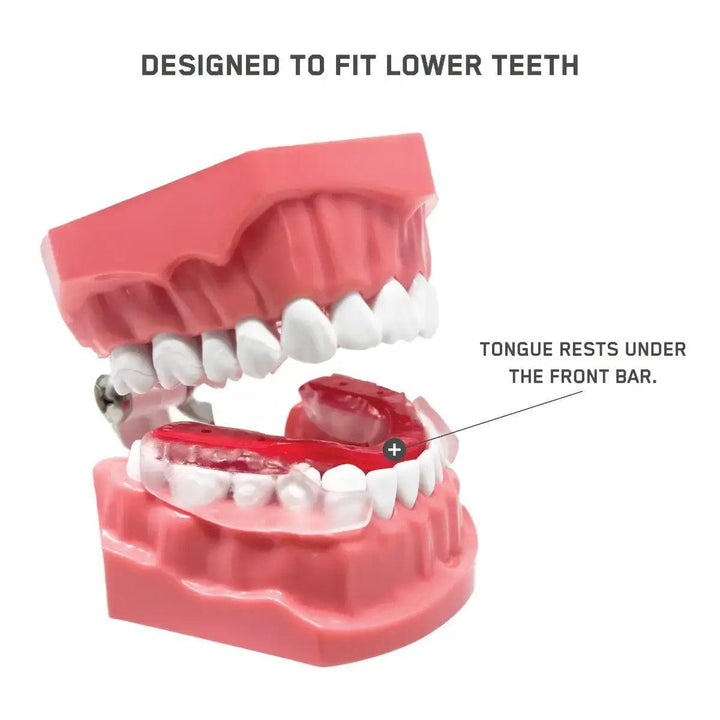
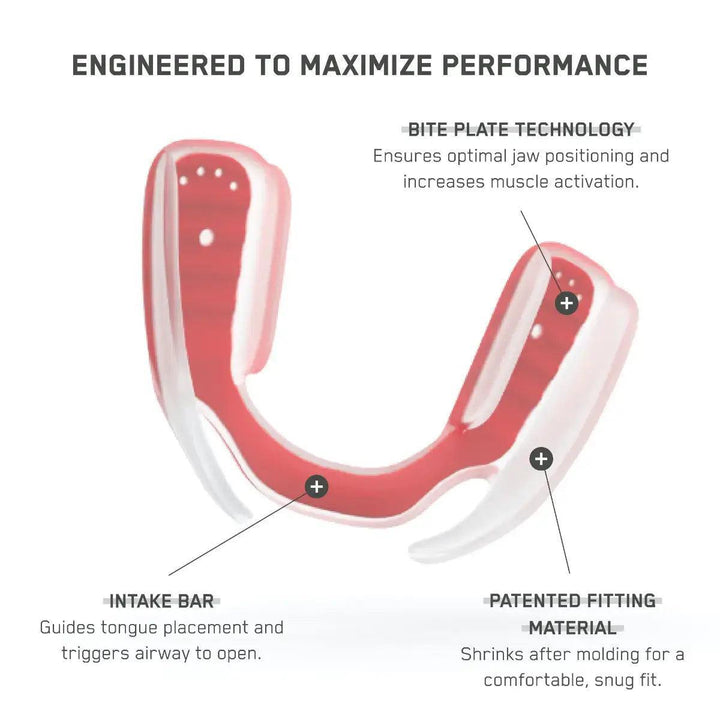
The AIRWAAV Recovery Mouthpiece is designed to support more consistent breathing during sleep. It fits on the lower teeth and uses gentle tactile cues that encourage the tongue to stay forward, helping maintain a more stable airway environment as muscle tone decreases.
This approach is built on more than 15 years of research into oral appliance design and human performance. The original research behind AIRWAAV’s mouthpiece technology was led by Dr. Dena Garner, a professor of Health and Human Performance at The Citadel with advanced training in muscle physiology, exercise physiology, and neurology.
That research foundation informs how oral positioning can influence recovery related metrics, including sleep architecture and physical recovery.
By improving breathing consistency during sleep, many users see:
-
Longer, more continuous deep sleep
-
Lower sleep stress
-
Improved HRV trends
-
Reduced physical fatigue
-
More predictable recovery
Why This Improves Physical Recovery Without More Sleep
Deep sleep is not about more hours. It is about fewer interruptions.
When breathing remains stable and the nervous system feels safe, the body can stay in deep sleep long enough to complete its recovery processes.
That leads to better physical resilience, faster adaptation, and more consistent performance within the same sleep window.
The Takeaway
Deep sleep is the engine of physical recovery. When it is interrupted, recovery suffers even if total sleep time is adequate.
One of the most common reasons deep sleep is disrupted is breathing inconsistency during sleep. These disruptions are often subtle and unnoticed, but their impact is real.
Supporting breathing stability helps protect deep sleep, allowing the body to complete the recovery work it is designed to do each night.